The ‘astounding’ rise of semaglutide — and what’s next for weight-loss drugs
Article meta
- Article Date: 2026-02-12
- Article URL: https://www.nature.com/articles/d41586-026-00228-1
- Article Title: The ‘astounding’ rise of semaglutide — and what’s next for weight-loss drugs
- Article Image:
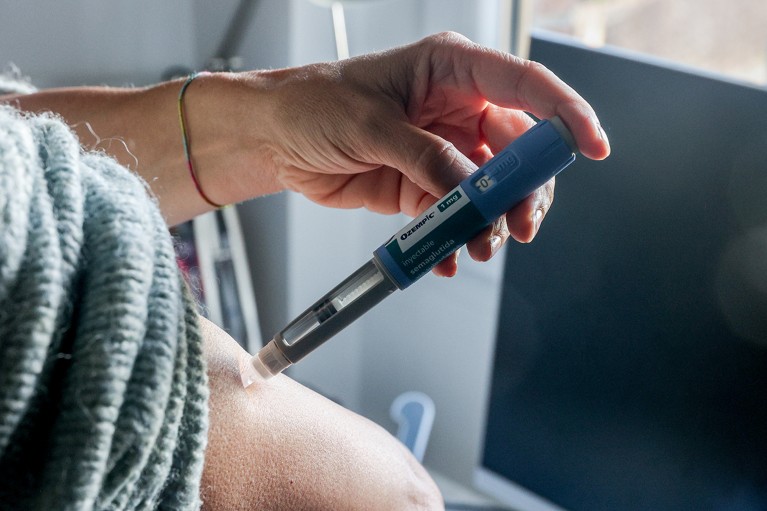
Summary
Semaglutide — a GLP-1 receptor agonist originally developed for type 2 diabetes — has rapidly become a leading treatment for weight loss, showing unprecedented results in clinical trials and drawing huge public attention. Originating from research into a peptide in Gila-monster venom and developed by Novo Nordisk into a longer-acting drug, semaglutide (marketed as Ozempic and Wegovy) produces significant and sustained weight reduction for many patients, along with improvements in diabetes control and some cardiovascular and kidney outcomes.
Trials such as STEP 1 found that weekly semaglutide injections enabled more than half of participants to lose at least 15% of body weight over 68 weeks. The drug is reshaping therapeutic approaches to obesity and has spurred a fast-moving pipeline of combination agents and multi-receptor agonists aiming for greater efficacy, better tolerability and oral formulations.
Key Points
- Semaglutide, developed from GLP-1 research, has produced large, clinically meaningful weight loss in multiple trials (e.g. STEP trials).
- Originally approved for type 2 diabetes (Ozempic), semaglutide later gained approval for weight loss (Wegovy) after strong obesity trial results.
- Mechanisms likely include appetite suppression via the arcuate nucleus and modulation of reward pathways, though details remain incompletely understood.
- Use of GLP-1 receptor agonists for obesity surged (~700% in US between 2019–2023), driven by public attention and celebrity endorsements.
- Access and cost are major issues: high prices and insurance gaps risk widening health inequalities, since early uptake has favoured those with private insurance.
- Stopping treatment often leads to weight regain, implying many patients may need long-term therapy similar to statins or blood-pressure drugs.
- Pharma competition is intense: dual and tri-agonists (e.g. tirzepatide, retatrutide), combinations like CagriSema, and adjuncts to preserve muscle are in trials to improve efficacy and tolerability.
- Broader societal questions remain: medicines do not address structural drivers of obesity and could affect attitudes towards body diversity and fat acceptance.
Content summary
The article traces semaglutide’s journey from peptides discovered in Gila-monster venom through successive drug development steps to create a long-acting GLP-1 agonist. Clinical research showed unexpected weight-loss benefits, prompting trials specifically for obesity and regulatory approval for that indication. Results across multiple studies demonstrate substantial weight reductions and additional health benefits for some complications of obesity and diabetes.
Researchers highlight likely brain-mediated appetite and reward effects, while clinicians report life-changing outcomes for many patients. At the same time, experts raise concerns about long-term use, cost, equitable access, and the limits of drugs as a solution to socio-economic drivers of obesity. The commercial race has shifted to tolerability, delivery (oral vs injectable) and combining mechanisms to push weight loss further.
Context and relevance
This article is important for clinicians, policymakers, industry watchers and the public because semaglutide is altering how obesity is treated and financed. It sits at the intersection of medicine, public health and social policy: huge clinical benefits for some, but also large cost and access challenges that could deepen inequalities. The rapidly expanding pipeline means more powerful therapies are coming, which will amplify debates about long-term use, regulation, reimbursement and societal attitudes to body weight.
Why should I read this?
Look — if you want a concise, evidence-focused take on why semaglutide matters (and why everyone’s talking about it), this is the article. It explains where the drug came from, what the major trials actually showed, how it works in the brain in plain terms, and why access and long-term policy choices are now urgent. Saves you time and gets you up to speed fast.
Author style
Punchy: the piece highlights transformative clinical results and frames semaglutide as a potential medical landmark while not shying away from the economic, ethical and social questions it raises. If you care about health policy or clinical practice, the article’s relevance is amplified — it’s not just new science, it’s a shift that will ripple through healthcare budgets, prescribing habits and public discourse.

